Iron is an essential mineral for making haemoglobin, a protein that carries oxygen around the body and gives the red blood cells their distinctive red colour. Low iron levels lead to low haemoglobin levels which may cause paler skin and lower levels of oxygen in the body, which may result in tiredness, lack of energy, shortness of breath (4).
Detecting low iron levels in time is important to prevent iron deficiency anaemia, which is estimated to occur in 9% of girls aged 11-18 years and 5% of women aged 19-64 years in the UK (1).
Possible symptoms of Iron deficiency
There are a variety of symptoms that may occur due to iron deficiency. These include: headaches, painful open sores or ulcers in the corners of your mouth, spoon-shaped nails, hair loss, feeling itchy and restless legs syndrome (4).
Iron is also important for a healthy immune system, thus frequent colds and/or infections are often seen in individuals with iron deficiency.
Causes of Iron deficiency
As 70% of the iron in adults is found in the red blood cells, iron deficiency is mainly associated with blood loss. In women of childbearing age, blood loss due to heavy periods is the most common cause of iron deficiency. One in 20 women aged 30-49 years in the UK consult their GP each year about heavy periods (3).
Other causes of severe blood loss leading to iron deficiency are stomach ulcers, piles, inflammatory bowel disease, and taking non-steroidal anti-inflammatory drugs such as ibuprofen and aspirin (4).
A diet low in iron also increases the risk of iron deficiency.
Iron requirements
Men and women have different requirements for iron. From the onset of menstruation until monthly periods stop, after the menopause, women need almost twice as much dietary iron as men. This is because menstruation (a woman’s monthly period) can use up the body’s iron stores, especially if dietary iron is low or if the woman has heavy periods. You can see the Reference Nutrient Intake (RNI) for adults below (5):
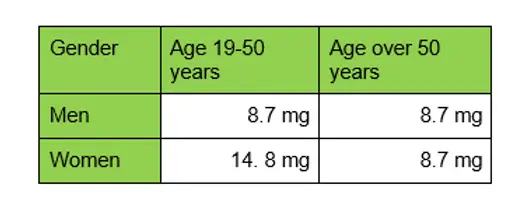
Women aged between 19 and 50 years have higher iron requirements than men, which place them on a higher risk of iron deficiency. Results from the UK’s National Diet and Nutrition Survey shows that 25% of women aged 19-64 years and 49% of girls aged 11-18 years have low iron intakes. In comparison, 2% of adult men and 11% of teenage boys are likely to have inadequate iron intakes (6).
Iron requirements are higher in pregnancy. A woman’s body adapts when pregnant and breastfeeding to ensure the baby receives an adequate supply of iron, even when the mother is iron deficient (7). Some pregnant women may develop low iron status, so plenty of iron-rich foods should be eaten. It can take several months for a woman to replenish her iron stores after a pregnancy. Leaving a gap of a year and a half between pregnancies has been suggested to enable nutrient stores to replenish (7).
How to optimise iron from your diet
Below are 6 tips to help you get more iron from your diet.
- Eating red meat a few times a week (for example a beef stir fry, mince or stew) provides a source of iron that is easily absorbed by the body.
- Including a variety of plant-based foods that provide iron. These include: dark green leafy vegetables (spinach, kale), nuts and seeds, fortified cereals, bread, dried fruit, and pulses (beans, peas and lentils)(4)
- Eating foods containing vitamin C (most fruit and vegetables, especially berries, tomatoes, peppers, Brussel’s sprouts, and broccoli) which enhance iron absorption during meals. This is especially important if your sources of iron are mainly plant-based, which are not as readily absorbed by the body as the iron found in animal sources.
- Don’t drink tea or coffee with a meal. Leave a gap of at least an hour between drinking tea or coffee and eating a meal as these drinks contain polyphenols such as tannins which reduce iron absorption from plant foods.
- Include iron-fortified foods such as fortified breakfast cereals. Drinking a small glass of fruit juice along with the cereal or adding some fresh berries on top will provide some vitamin C to enhance the absorption of the iron.
- Use cast iron pots to cook your meals. Evidence suggests that tiny amounts of iron from the pots leach into the food during cooking, so they can help reduce iron-deficiency anaemia (8).
In circumstances where optimal iron levels cannot be achieved through diet, an iron supplement may be prescribed by your GP.





